Our body harbors trillions of tiny microscopic organisms called microbes. Collectively, all the microorganisms — bacteria, viruses, fungi, and other life forms that live in our bodies are known as the microbiome.
Various organs in our body have distinct microbial populations. Microflora is the term used to describe the collection of organisms that live together in a certain habitat. The microflora that lives in our digestive tracts is “gut flora,” or microbiota.
Our gastrointestinal tract has the largest population of microbiota. Microbes can also be found in the nose, small intestine, mouth, throat, skin, lungs, and vagina.
According to researchers, approximately 100 trillion microbes exist in the human gastrointestinal tract or the gut. Among them are 1,000 different species of bacteria and also some viruses, fungi, and protozoa.
The human genome consists of about 23,000 genes, whereas the microbiome is more genetically complex, encoding over three million genes. In fact, in the human body, the microbial cells exceed human cells by 10 to 1.
The gut microbiota composition is unique to each individual and generally remains stable throughout life. Simply speaking, the microbiota in our intestine is as unique as our fingerprint; it acts like an individual identity card.
The gut microbiota plays a role in the digestion of food and affects the immune system, central nervous system, and other bodily processes.
Gut microbes also help in absorption and synthesis of nutrients.
These microbes play a crucial role in helping maintain our health. However, to do so, the gut microbiota has to remain in perfect balance. When the balance of this gut flora is disturbed, it can lead to health problems. Thus, the presence of gut microbiota is crucial for our well-being and health.
Composition of the Gut Microbiota
A diverse population of microorganisms makes up the gut microbiota. In addition to bacteria and viruses, the microbiota is made up of archaea (single-celled microorganisms) and unicellular eukaryotes (e.g., yeast and protozoa).
But bacteria make up the majority of the gut population. Some of the gut bacterial genera include Bacteroides, Lactobacillus, Escherichia, Bifidobacterium, Eubacteria, Actinobacteria, Clostridium, Prevotella, and Fusobacterium. Proteobacteria, Firmicutes, Actinobacteria, and Bacteroidetes make up 93% of the gut microbiota.
The structure and environment of the gut determine the type of microbial habitat. Basically, the environmental conditions (e.g., pH levels fluctuate through the gut) in the human gut are not uniform i.e., the human stomach and the colon have different environments.
So, microbial populations vary based on their location in the gut. Based upon their location in the gut, the microbes differ in several features including composition, cell density, and metabolic activity.
The gut microbiota plays a vital role in the synthesis of enzymes, vitamins (vitamin K and vitamin B) and amino acids, and nutrient and mineral (magnesium, calcium, and iron) absorption. It helps in digestion, provides protection against pathogens, and shapes your mood and behavior.
The evidence is mounting of the gut microbiota’s health significance. Several studies have shown a strong association between gut microbiota and many human diseases.
There are several factors that influence the gut microbiota composition. Diet, nutrition, exposure to stress, environment, and medications are some of them. Disruption or imbalance in the gut microbiota is called dysbiosis.
Research has revealed growing evidence of the role of diet in modulating the composition and metabolic activity of the human gut microbiota, which in turn can impact health. Several experiments have shown that changes to diet can cause significant but temporary changes in microbiota within 24 hours.
Gut microbes produce a large number of bioactive compounds that can influence health; some like vitamins are beneficial, but some products are harmful. The maintenance of a diverse and thriving population of beneficial gut bacteria is essential to keep harmful bacteria.
How does the Gut Microbiota Develop?
Your gut gets colonized by microbes very early in life. It was earlier thought that the mother-to-child transfer of microbiota occurs at birth; however, some scientific studies suggest that the first exposure to bacteria happens few hours or even less before birth (through the placental barrier).
After the birth, many factors influence the microbial population that will live and thrive in your gut – the genetics and health of your parents, delivery mode (whether you are delivered vaginally or by cesarean), and mode of feeding (whether you are breast or bottle-fed).
The intestinal microbiota of infants is low in diversity but becomes more diverse as time after birth increases. By the end of the first year of life, infants have an individually unique microbial flora. With increasing age, microbial diversity increases by the incorporation of new bacterial taxa. By 2–5 years of age, the microbiota in children fully resembles that of an adult with respect to composition and diversity.
The microbiota tends to remain relatively stable throughout adult life; however, many factors shape the bacteria that live in your gut. Genetics, illness, diet, and lifestyle affect the composition of the microbiota.
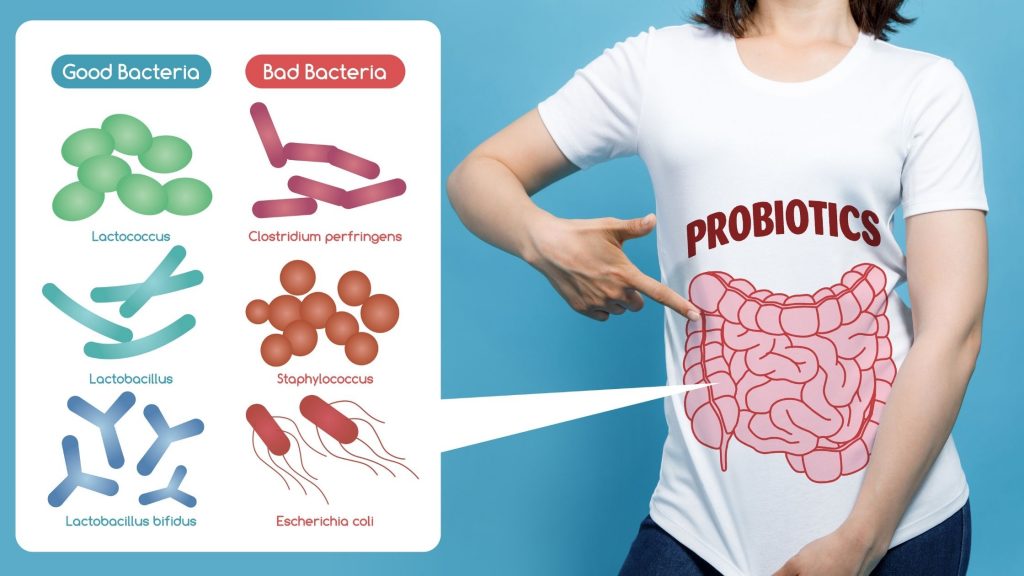
A healthy gut has ‘good’ bacteria that assist in the physiological functions of the body. The ‘good’ bacteria also keep you protected from the ‘bad’ bacteria. But when the balance of the gut microbiota gets disturbed, the ‘bad’ bacteria take over.
These ‘bad’ bacteria have the potential to ruin your health. So, looking after your gut microbiota through a healthy diet and active lifestyle is the best way to good health and well-being.
Diet and Gut Microbiota
Diet can be considered as the primary factor influencing gut microbiota composition and function.
Our dietary habits largely determine the type of bacteria that live and flourish in the gut. Complex interactions between nutrients (present in our food) and microorganisms determine beneficial or harmful outcomes to human health.
The human diet primarily contains proteins, fats, and carbohydrates. The type and amount of these primary components influence the composition of the gut microbiota.
Microbial metabolism of dietary carbohydrates results mainly in the formation of short-chain fatty acids (SCFAs). The formation of SCFA’s (acetate, propionate, and butyrate) is an excellent example of the symbiotic relationship between humans and gut bacteria.
Carbs provide a critical energy source for gut bacteria, and SCFAs help lower the pH within the colon. Butyrate is a primary energy source for colonocytes and also maintains intestinal homeostasis.
An increase in dietary fat also significantly alters microbiota composition. For example, it has been shown that a high-fat diet adversely reduces A. muciniphila and Lactobacillus, which are both associated with healthy metabolic states.
Proteins are an essential part of a balanced diet. However, excess protein in a diet can disturb the microbiota. The metabolites that are produced after a high-protein diet are potentially harmful to colonic health.
Dietary patterns also influence microbial inhabitants in the gut. A study found that people who eat a primarily plant-based diet, such as vegans and vegetarians, had a dominance of Prevotella and lacked in Bacteroides.
On the other hand, those who consumed meat had an abundance of Bacteroides. Vegetarians who consumed an animal-based diet for four days had their Prevotella-to-Bacteroides ratio inverted.
Furthermore, traditional diets high in fresh and whole foods and include minimally processed foods give rise to a diverse gut microbial population.
The Western diet, which is typically high in fat and refined carbohydrates, decreases overall microbial diversity.
Gut Microbiota in Health
Gut microbiota is essential for humans to maintain optimal health. It regulates metabolism and supports nutrition and immune response. Changes in dietary habits and long-term consumption of processed food/junk food can cause changes to the gut microbiota, affecting your health.
More than 50% of alteration of gut microbiota has been linked to dietary habits of the individuals. You can do several things to improve your gut bacteria and resolve non-beneficial effects in the human body.
Take probiotics
Probiotics are live microorganisms that offer certain health benefits when consumed. They are present in yogurts and certain fermented foods and also as food supplements. Probiotics help restore a healthy gut microbiome.
Eat fermented foods
Fermented foods also contain live microorganisms; fermented foods are foods altered by microorganisms. Kimchi, sauerkraut, kombucha, tempeh are some fermented foods which are good for gut health.
Eat prebiotics
Prebiotics promote the growth of beneficial microbes in the gut. Many fruits, vegetables and whole grains contain prebiotics. Prebiotics can be added to yogurts, cereals, or breads.
Eat whole grains, plants, fresh fruit, and veggies
Grains like barley, quinoa, oats, and bulger have fiber which is great for digestion. Fresh vegetables, beans, legumes, and fresh fruits have lots of fiber in them, and they promote the growth of certain beneficial bacteria.
Eat foods rich in polyphenols
Polyphenols are micronutrients that are present in certain plant-based foods. They offer health benefits like lowering blood pressure, inflammation, and oxidative stress. Nuts, seeds, green tea, cocoa, dark chocolate, broccoli, and berries are polyphenol-rich foods.
They feed the Bifidobacteria in your gut, thereby increasing the population of these bacteria. This promotes the health of your gut.
Limit your sugar intake
Food and beverages high in sugar harm the gut microbiota; increased sugar intake disrupts the metabolism of microbes and reduces gut diversity. Artificial sweeteners negatively influence blood glucose levels by disrupting the gut flora. Best to avoid sugary foods altogether.
Gut Microbiota in Disease
A healthy gut is a diversely-populated gut, and eating a wide range of healthy foods is the best way to build a diverse microbiota.
A diverse microbiota also keeps diseases at bay and lowers the risk of allergies. In recent years, there is increasing evidence supporting an association between gut microbiota and diseases in humans.
Research indicates that the alteration of gut microbiota may contribute to developing a range of CVDs from atherosclerosis to cardiorenal dysfunction.
Disruption of the gut microbiome, generally associated with loss of microbial diversity, may contribute to a range of chronic diseases, including obesity, multiple sclerosis, and autism spectrum disorders (ASD). The development of type 2 diabetes mellitus is also linked to gut microbiota disturbance.
Disturbances in the composition and function of gut microbiota have been implicated in various forms of inflammatory bowel diseases (IBD), including Crohn’s disease (CD) and ulcerative colitis.
Gut Microbiota as A Therapeutic Target
With research indicating an increasing role of diet in maintaining a healthy gut microbiota which in turn helps in keeping diseases at bay, dietary interventions might potentially be used to manage complex diseases.
Disruption in gut microbiota can be used as biomarkers for early detection of disease risk and opportunities for preventive interventions.
For example, recently, the fecal microbiota transplant was used effectively to manage several different conditions, including ulcerative colitis, Clostridium difficile-associated colitis, irritable bowel syndrome, and even obesity. Dietary intervention and microbial supplementation were also used successfully to restore the gut microbiota balance and treat some conditions.
These efforts show that the gut microbiota represents a viable therapeutic target for disease management, prevention, and cure.
Conclusion
The gut microbiome comprises trillions of microorganisms that co-exist with other human cells in the human gastrointestinal tract or gut.
This gut flora aids in digestion and metabolism and supports immune functions and brain health. Our gut microbiota begins to develop very early in life and is influenced by genetics, delivery method, feeding method, age, illness, diet, and other environmental factors.
Diet is a key factor that influences the number and diversity of the human gut microbiota. Poor dietary habits and lifestyle can cause changes in the gut microbiota leading to several health problems.
Adopting a healthy diet which involves eating fresh veggies, fruits, whole grains, legumes and probiotics and prebiotics can help restore a healthy gut microbiota.
Dietary interventions that restore gut microbiota can help fend off many diseases.